The Question Every Patient Asks First
Deep Plane Facelift scars are the single most common anxiety patients bring into a facial rejuvenation consultation. There is one moment that follows the same quiet choreography in nearly every session. The patient reaches up, gathers her hair behind her ears, and asks the question that has clearly been on her mind for weeks: “If I go through with this, will I ever be able to wear my hair up again? Will people see the facelift scars around my tragus?”
It is a perfectly reasonable fear — and one that a skilled facelift surgeon takes as seriously as the surgery itself. The patient considering a Deep Plane Facelift wants to look like a refreshed, radiant version of herself, not to carry visible facelift scars behind her ears for the rest of her life. The ultimate measure of a world-class facelift is not how dramatic the transformation appears, but how completely the evidence disappears.
A board-certified plastic surgeon devotes as much precision to designing the incision architecture as to the internal tissue repositioning. The secret to truly undetectable facelift scars does not reside in a single elegant stitch. It begins far deeper — in the strategic release of facial ligaments, the meticulous elevation of the SMAS, the precision of the tragus incision, and the biomechanical principle that allows skin to heal without tension.
What follows is the full anatomy of how facelift scars are planned — from tragus incision design to hairline routing — and guided toward invisibility, along with an honest, science-based facelift recovery timeline of what your healing will actually look like.
The Tragus: Understanding the Anatomy That Hides Your Scars
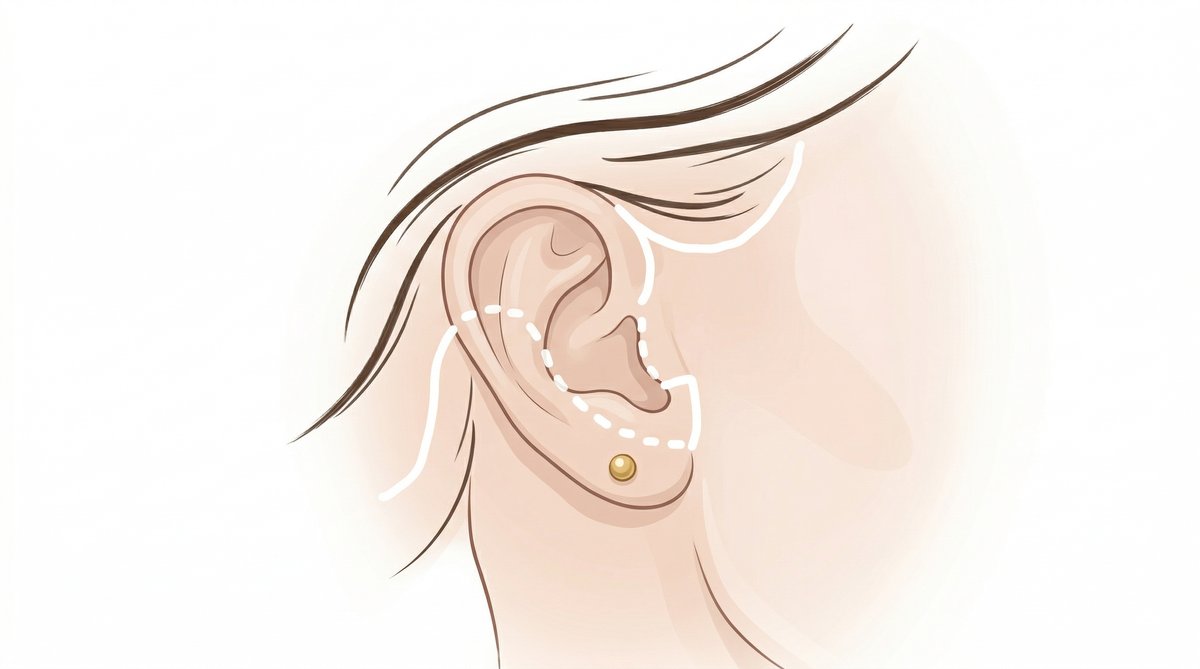
Before discussing incision strategy, you need to meet one small but remarkably important piece of your anatomy: the tragus. This is the firm, rounded flap of cartilage that sits directly in front of your ear canal. Run your fingertip over it right now — that small projection is the single most critical landmark in facelift scar concealment.
The tragus creates a natural shadow, a tiny architectural overhang where a skillfully placed incision can virtually disappear. How a surgeon navigates this structure — the precision of the tragus incision placement — determines whether your facelift scars remain invisible to the world or announce themselves under bright light.
When designing the tragus incision for a Deep Plane Facelift, the incision placement strategy follows one of two fundamentally different approaches. Each carries distinct advantages depending on your skin type, gender, and aesthetic goals.
Pre-Tragal vs. Retro-Tragal Incision: A Direct Comparison
| Feature | Pre-Tragal Incision (In Front of the Tragus) | Retro-Tragal Incision (Behind the Tragus Edge) |
|---|---|---|
| Placement | Traces the natural skin crease just anterior to the tragus cartilage. | Tucks inside the tragal rim, concealed within the ear’s own shadow. |
| Ideal Candidates | Men (to preserve the beard line), patients with deeper periauricular creases, and revision cases. | Women with smooth periauricular skin, younger patients, and anyone prioritizing maximum scar camouflage. |
| Visibility | Faintly perceptible in patients who lack deep natural skin folds around the ear. | Virtually invisible — hidden within the ear’s own contour and shadow anatomy. |
| Technical Demand | Well-established technique with lower risk of altering the tragal cartilage shape. | Highly advanced. Demands precise tension distribution to prevent flattening or distortion of the tragus. |
For female patients whose primary concern is an imperceptible scar — especially those who envision wearing their hair swept up, pinned back, or styled in a high ponytail — the retro-tragal approach is widely regarded as the gold standard in modern facelift incision placement. By hiding the incision within the ear’s own architectural contour, the visible footprint of surgery is reduced to virtually nothing.
Bespoke Incision Design: Why Your Unique Anatomy Dictates Every Cut
There is no universal facelift incision — and any surgeon who applies a one-size-fits-all template is ignoring the anatomical reality that makes each face unique. A masterfully executed Deep Plane Facelift — the procedure that has become the cornerstone of advanced Korean plastic surgery for facial rejuvenation — demands a bespoke surgical blueprint that accounts for the specific geometry of your ears, hairline, skin quality, and tissue volume.
Three anatomical variables deserve particular attention.
Earlobe Architecture and the Pixie Ear Risk
Examine your earlobes closely. Do they attach directly to the side of your jaw, or do they hang freely with a defined inferior border? This distinction profoundly influences how the incision must be designed and closed.
The incision must follow the precise natural curvature of your individual earlobe with meticulous fidelity. If a surgeon applies excessive tension to the skin flap during closure — or fails to account for the natural elasticity of the lobular tissue — the earlobe is gradually dragged downward and anteriorly over the ensuing months. The result is a telltale deformity known as the pixie ear: a thinned, elongated, pulled-forward earlobe that is one of the most recognizable signs of a poorly executed facelift.
Preventing pixie ear deformity is not a matter of luck. It is a matter of tension-free closure at the lobular junction — a principle that is inherently easier to achieve when the deep tissue layers, rather than the skin, bear the structural load of the lift. This is precisely where the Deep Plane technique offers its most significant advantage over skin-only or superficial SMAS approaches.
The Temporal and Occipital Hairlines: Engineering the Ponytail Facelift
For patients who envision confidently wearing a high ponytail, a sleek bun, or simply tucking their hair behind their ears without a second thought, the hairline incisions are just as critical as the periauricular ones.
In the temporal region (above and in front of the ear), the incision can be concealed within the hair-bearing scalp itself — an approach known as the intratrichial incision — or placed precisely at the anterior hairline border. The choice depends on your existing hairline density and whether any temporal recession would be undesirable.
Behind the ear, the incision ascends into the post-auricular sulcus (the deep crease where the ear meets the skull) before gracefully tapering into the occipital hairline at the back of the head. This posterior design is what makes the so-called ponytail facelift concept a reality: when every incision is meticulously routed through natural creases and hair-bearing tissue, you can pull your hair into any updo without revealing a trace of surgery.
The Male Facelift: Why Gender Changes Everything
Male patients require an entirely different incision philosophy — and this is a detail that separates experienced facelift surgeons from the rest.
During a facelift, the skin is redraped and repositioned. In a male patient, this means hair-bearing, beard-growing skin is shifted along with it. If a retro-tragal incision were used on a man, the redraping process would transport beard follicles directly onto the tragus and into the ear canal — creating the bizarre and uncomfortable necessity of shaving inside one’s own ear.
For this reason, male facelifts almost universally employ a carefully camouflaged pre-tragal incision, positioned to preserve the natural sideburn contour and the integrity of the shaving line. The incision is designed to sit within the deepest periauricular skin crease, where it can mature into an imperceptible fine line even without the added camouflage of the retro-tragal shadow.
Surgeon’s Insight: The Secret to Invisible Facelift Scars Isn’t the Suture — It’s the SMAS
A common misconception surfaces in consultations: the belief that beautiful facelift scars come down to a surgeon who is “good at stitching.” While meticulous, multi-layered suturing is absolutely non-negotiable, it is only the final chapter of a much longer story.
The true engineering of an invisible scar happens beneath the surface — in the deep plane itself.
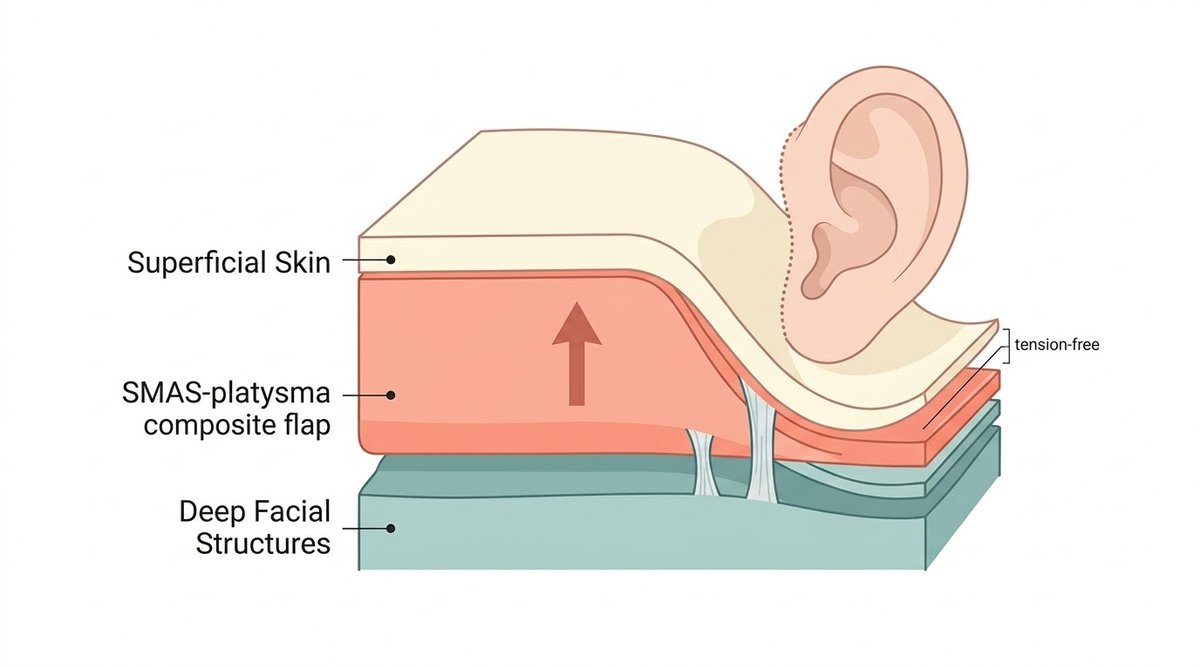
In a Deep Plane Facelift, the surgeon surgically releases the retaining ligaments of the face and elevates the SMAS as a unified composite flap. This deep structural layer — the actual architectural scaffolding of the face — is repositioned and secured into its new, elevated position. Because this robust internal framework is bearing one hundred percent of the lifting tension, the overlying skin simply redrapes over your restored contours with zero mechanical stress.
This is the biomechanical principle that separates a pencil-thin, invisible scar from a wide, thickened, hypertrophic one. When skin is closed under tension, the body responds by depositing excessive collagen at the wound margin, producing a raised, conspicuous scar. When skin is closed in a state of complete mechanical repose, the incision heals flat, soft, and — given time — virtually indistinguishable from the surrounding tissue.
The stitch closes the wound. The deep plane makes it disappear.
The Honest Healing Timeline: What Your Facelift Scars Will Actually Look Like
To be direct: every surgical incision produces a scar. There is no technology, no suture material, and no topical product that can eliminate this biological reality. What separates an exceptional result from a merely adequate one is not the absence of scarring but the maturation and camouflage of the scar — how quickly the scar healing progresses, how flat it remains, and how completely it integrates into the natural creases of your ear and hairline.
Your facelift scars will progress through four distinct biological phases. Understanding this timeline in advance is one of the most effective tools for maintaining confidence and peace of mind during your facelift recovery.
Days 1–7: The Inflammatory Phase
The incisions are fresh, precisely aligned, and protected by fine sutures. You will experience the expected swelling, bruising, and mild discomfort that accompany any surgical procedure. The incision lines may appear slightly raised and pink — this is entirely normal wound physiology. During this phase, your body is deploying its inflammatory cascade to seal the wound and lay the groundwork for tissue repair.
Weeks 2–4: The Proliferative Phase
Sutures are removed during this period. The incisions are closed and structurally stable, but they will appear pink, slightly firm to the touch, and occasionally feel mildly bumpy beneath the fingertip. This firmness is the result of new collagen being deposited at the wound site — a necessary and healthy part of tissue repair. Most patients find that simply wearing their hair down is more than sufficient to conceal the healing incisions during this brief window.
Months 1–3: Neovascularization and the Redness Peak
This is the phase that unsettles patients most — and the one that experienced facelift surgeons spend the most time discussing during preoperative consultations, precisely because it is the most misunderstood.
During months one through three, you may notice that your scars suddenly appear more red, more pink, or more prominent than they did just weeks earlier. This is not a complication. It is a biological process called neovascularization — your body is constructing thousands of microscopic new blood vessels to deliver oxygen, nutrients, and growth factors to the healing tissue. The increased blood flow is what produces the redness, and it is a sign that your body’s repair machinery is operating exactly as it should.
The redness is temporary. It is purposeful. And it will resolve.
Months 6–12: Maturation and the Vanishing Act
This is when the true artistry of the surgical plan reveals itself. The temporary blood vessels that served the healing process gradually recede. The intense redness fades week by week. The collagen fibers remodel from a disorganized repair matrix into an aligned, supple tissue structure. The scar softens, flattens, and progressively blends into your natural skin tone until it becomes what every patient hopes for — a barely perceptible, pale fine line concealed within the natural shadows of your ear anatomy and hairline.
By the twelve-month mark, the overwhelming majority of patients report that even they have difficulty locating their own scars.
Your Role in the Healing Process: Proactive Scar Management
While surgical technique is the single most influential determinant of scar quality, your aftercare protocol plays a meaningful supporting role. These are the three evidence-based interventions recommended to every patient.
Shield every incision from ultraviolet exposure. A healing scar is acutely vulnerable to UV-induced hyperpigmentation — a darkening that can become permanent if the tissue is exposed to direct sunlight before it has fully matured. Once the incision lines are completely closed and cleared by the surgical team, apply a broad-spectrum SPF 50+ sunscreen directly along every external incision, every day, without exception.
Begin medical-grade silicone therapy when cleared. Silicone gel or silicone sheeting is the single most well-documented topical intervention for scar optimization. It functions by maintaining hydration at the wound surface, which signals the underlying fibroblasts to moderate their collagen production. The result is a flatter, softer, less conspicuous scar. Begin use only after explicit clearance from your surgical team.
Ask about advanced scar therapy if needed. For patients with keloid-prone skin or scars that remain raised beyond the expected timeline, in-clinic interventions such as fractional laser resurfacing, steroid micro-injection, or pulsed-dye laser treatment can accelerate maturation and flatten persistent scar tissue. These are reserved for the small minority of patients whose biology requires additional support beyond standard aftercare.
Eliminate nicotine entirely. This is not a suggestion — it is a clinical imperative. Nicotine constricts the microvasculature, reducing oxygen delivery to the healing tissues by a significant margin. The consequences can range from widened, discolored scars to severely delayed scar healing and, in extreme cases, skin flap necrosis. If you are considering a Deep Plane Facelift, complete nicotine cessation is a non-negotiable prerequisite for safe candidacy.
Confidence, Restored
A beautifully executed Deep Plane Facelift should leave you looking like the most rested, luminous, and gravity-defying version of yourself — without leaving behind the visual evidence of a surgeon’s work. By engineering the incision to your specific anatomical landmarks, placing every cut within the natural shadows and creases of the ear and hairline, and harnessing the tension-free biomechanics of the deep plane, the goal is not merely improvement but imperceptibility.
You will wear your hair up. You will tuck it behind your ears. And the only thing anyone will notice is how remarkably well you look.
Curious how the Deep Plane technique compares to the traditional approach? Read the in-depth analysis of Deep Plane Facelift vs. SMAS: which procedure is right for you. If unnatural results are your primary concern, explore why the windblown look happens and how the Deep Plane prevents it.
Written by Dr. Yongwoo Lee, board-certified Korean plastic surgery specialist in facelift and anti-aging surgery at VIP Plastic Surgery, South Korea.
Frequently Asked Questions About Deep Plane Facelift Scars
Where exactly are deep plane facelift scars located?
Deep Plane Facelift incisions are strategically placed in three zones designed for maximum concealment. The temporal incision hides within or along the hairline above the ear. The periauricular incision traces the natural contour of the ear, either in front of the tragus cartilage (pre-tragal) or tucked behind its edge (retro-tragal). The posterior incision ascends into the crease behind the ear before tapering into the occipital hairline. When each segment is precisely positioned within natural anatomical creases and hair-bearing tissue, the resulting scars become virtually undetectable once they have fully matured.
How long does it take for deep plane facelift scars to fade?
Facelift scars progress through a predictable biological timeline. During the first one to three months, the scars may appear red or pink due to neovascularization, the body’s natural process of building new blood vessels to support tissue repair. This redness gradually subsides over months three through six. By the six-month mark, most scars have faded significantly, and by twelve months, the majority have matured into fine, pale lines that blend seamlessly with the surrounding skin. Individual healing varies depending on genetics, skin type, and adherence to aftercare protocols.
Can I wear my hair up in a ponytail after a deep plane facelift?
Yes, and this is one of the most important goals of modern incision design. By routing the temporal incision within or along the hairline and concealing the posterior incision in the post-auricular sulcus before it transitions into the occipital hair, every scar is hidden beneath hair-bearing tissue. Once the incisions have healed and matured, typically by three to six months, patients can confidently wear high ponytails, buns, and updos without revealing any surgical evidence. This capacity is sometimes referred to as the ponytail facelift standard of scar concealment.
What is pixie ear deformity and how is it prevented?
Pixie ear deformity is a telltale sign of a poorly executed facelift in which excessive tension on the skin flap gradually pulls the earlobe downward and forward, producing an elongated, thinned, unnatural appearance. It occurs when the skin rather than the deeper structural layers is forced to bear the mechanical load of the lift. In a Deep Plane Facelift, the retaining ligaments and SMAS layer carry the entirety of the lifting tension, which allows the skin to be closed over the earlobe with zero mechanical stress, preserving the natural lobular contour and preventing the distortion that causes pixie ear.
Do deep plane facelift scars look different from traditional SMAS facelift scars?
The incision locations are similar, but the quality of the resulting scars can differ meaningfully. In a traditional SMAS facelift, a greater proportion of the lifting tension is distributed through the skin closure, which increases the risk of wider, more conspicuous scars and earlobe distortion over time. In a Deep Plane Facelift, the deep tissue layers absorb the full mechanical load, enabling a completely tension-free skin closure. This biomechanical advantage consistently produces thinner, flatter, and less visible scars that mature more favorably over the twelve-month healing period.
Why do facelift scars sometimes become more red before they fade?
The temporary increase in redness that many patients observe between months one and three is caused by neovascularization, a normal and essential phase of wound healing. During this period, the body generates thousands of microscopic new blood vessels to supply the healing tissue with oxygen, nutrients, and repair-facilitating growth factors. The concentrated blood flow is what produces the visible redness and occasional slight elevation of the scar. This process is not a complication but rather a sign that the body’s tissue repair system is functioning optimally. The excess vasculature gradually recedes as the scar matures, and the redness fades progressively over the following three to nine months.
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified medical professional before making any decisions about surgical or non-surgical procedures.